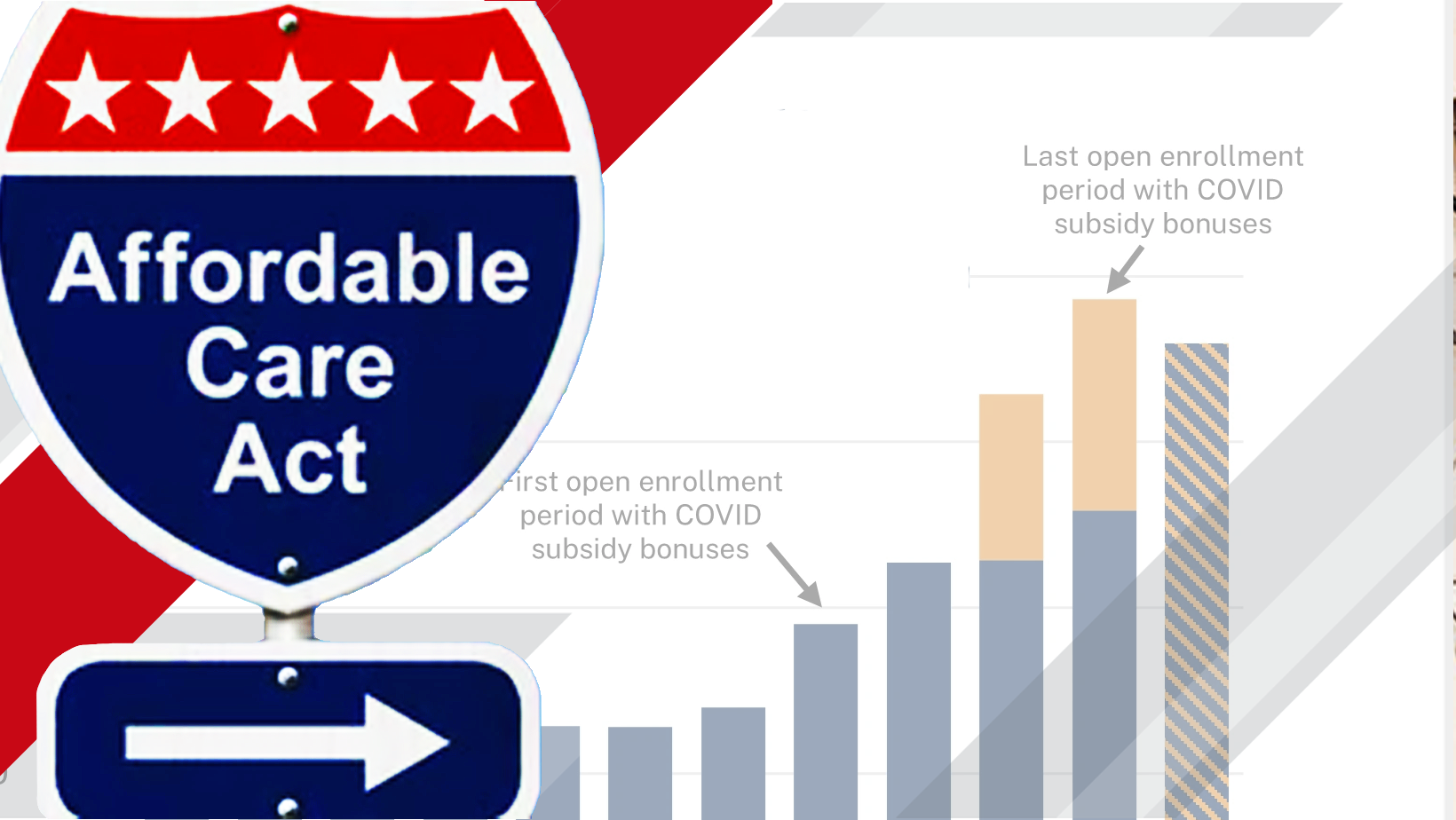
Impact of ACA Premium Payment Trends on Enrollment and Insurers
Rising premium pressure and shifting enrollment behavior are quietly reshaping the ACA marketplace in ways that demand immediate attention from insurers and agents alike.
Recent data highlights a meaningful shift in Affordable Care Act participation patterns, with approximately 14% of enrollees failing to pay January premiums. While enrollment totals may appear relatively stable at first glance, the underlying dynamics tell a more complex story that carries real implications for carriers, agencies, and policyholders.
The expiration of enhanced tax credits tied to pandemic-era relief has created a sharp affordability cliff. For many subsidized consumers, premiums have more than doubled in 2026, fundamentally altering purchasing behavior and retention patterns across the exchange population.
A Hidden Enrollment Decline
Headline enrollment figures suggest only a modest 5% drop year over year. However, payment behavior reveals a deeper contraction. When factoring in non-paying members, actual enrollment declines may range between 17% and 26%.
This gap between reported enrollment and active coverage is critical. Agents and carriers relying solely on enrollment data may be overestimating the stability of their ACA book of business.
“Enrollment numbers alone do not tell the full story. Payment behavior is where the real market signal lives.”
Health Policy Analyst
For agencies, this means rethinking how success is measured. Retention is no longer just about renewals. It is about ensuring clients can and will maintain coverage month to month.
Why Premium Shock Is Driving Behavior
The removal of enhanced subsidies has disproportionately impacted middle-income enrollees who previously benefited from expanded eligibility thresholds. Without those supports, many consumers are now facing premiums that exceed their perceived value of coverage.
This has led to a predictable but important shift. Healthier individuals are more likely to exit the market, while those with higher expected medical needs are more likely to remain.
That imbalance introduces risk across the entire ACA ecosystem.
State-Level Differences Are Becoming More Pronounced
Not all markets are experiencing these changes equally. States operating their own exchanges have demonstrated stronger premium payment rates, largely due to localized outreach efforts and supplemental financial assistance programs.
Meanwhile, states with less robust reenrollment systems or higher premium increases are seeing more significant drop-off.
For carriers and agencies operating across multiple states, this creates a fragmented operating environment where strategy must be tailored market by market.
Morbidity Trends Signal Rising Costs
Perhaps the most important development is the shift in the risk pool. Remaining enrollees are, on average, 10% more morbid than those who exited due to nonpayment.
Projected morbidity increases of 2.9% to 6.5% in 2026 suggest that claim costs will rise, putting upward pressure on future premiums.
This dynamic creates a feedback loop. Higher premiums drive healthier individuals out, which increases costs, which then drives premiums even higher.
“When healthier members leave, the math changes quickly. Carriers must adjust or absorb significant risk.”
Actuarial Consultant
What This Means for Carriers and Agencies
The current environment introduces both operational challenges and strategic opportunities. Organizations that adapt quickly will be better positioned to manage volatility and protect profitability.
Key Considerations Moving Forward
- Retention Focus: Proactively engage clients to prevent premium nonpayment and coverage lapses.
- Market Segmentation: Adjust strategies based on state-specific dynamics and payment trends.
- Pricing Strategy: Prepare for upward rate pressure driven by higher morbidity.
- Consumer Education: Help clients understand subsidy changes and plan for affordability shifts.
- Risk Management: Monitor claims experience closely to avoid misaligned pricing assumptions.
ACA Market Snapshot
| Metric | Insight |
|---|---|
| Enrollment Change | Reported decline modest Actual active coverage drop significantly higher |
| Premium Impact | Subsidy loss drives Average net premiums more than doubling |
| Risk Pool | Higher morbidity among Remaining enrollees increases claims pressure |
Navigating the Road Ahead
The ACA marketplace is entering a period of recalibration. While the system is not experiencing the extreme contraction once predicted, the structural changes underway are significant.
For agents, this is a moment to deepen client relationships and reinforce value beyond enrollment. For carriers, it is a test of pricing discipline, risk management, and market agility.
Those who recognize the difference between enrollment numbers and active, paying membership will be better equipped to respond to what comes next.